HEALTH
The Hidden Benefits of Personalised Oral Health Strategies

Understanding the Revolution in Dental Care
The landscape of dental care has undergone a remarkable transformation over the past decade, moving away from the traditional one-size-fits-all approach towards bespoke oral health solutions. A private dentist Manchester understands that this shift represents more than merely a trend; it embodies a fundamental understanding that each person’s mouth is as unique as their fingerprint, requiring tailored strategies to achieve optimal results.
Modern dental professionals have embraced the concept that personalised care extends far beyond routine check-ups and standard treatments. By considering factors such as genetics, lifestyle habits, dietary preferences, and individual risk factors, practitioners can develop comprehensive strategies that address the root causes of oral health issues rather than simply treating symptoms as they arise.
The Science Behind Individual Oral Ecosystems
Every mouth harbours a distinct bacterial ecosystem, influenced by numerous factors including saliva composition, pH levels, and genetic predispositions. Research has demonstrated that what works brilliantly for one patient may prove entirely inadequate for another, even when presenting with seemingly identical symptoms or conditions.
This biological diversity explains why some individuals can consume sugary treats with minimal consequences whilst others develop cavities despite meticulous oral hygiene routines. Understanding these nuances allows dental professionals to create targeted interventions that work harmoniously with each patient’s natural oral environment, leading to more effective and sustainable outcomes.
Tailored Prevention Strategies
Risk Assessment and Early Intervention
Personalised oral health strategies begin with comprehensive risk assessments that evaluate multiple factors contributing to dental problems. These evaluations consider medical history, current medications, hormonal fluctuations, stress levels, and occupational hazards that might affect oral health. By identifying potential issues before they manifest, practitioners can implement personalised preventive care approaches that significantly reduce the likelihood of future complications.
Customised Home Care Regimens
Gone are the days when dental professionals would recommend identical brushing and flossing routines to every patient. Modern personalised approaches involve selecting specific toothpastes, mouthwashes, and oral care tools based on individual needs. For instance, patients with sensitive teeth might benefit from specialised formulations, whilst those prone to tartar buildup require different interventions entirely. A private dentist in Manchester might recommend electric toothbrushes with specific brush head designs for patients with dexterity issues, or prescribe particular fluoride concentrations based on cavity risk assessments.
Advanced Diagnostic Technologies
The integration of cutting-edge diagnostic tools has revolutionised how dental professionals assess and monitor oral health. Digital imaging, genetic testing, and bacterial analysis provide unprecedented insights into individual oral health patterns. These technologies enable practitioners to identify predispositions to gum disease, assess bone density variations, and detect early signs of oral cancer with remarkable precision.
Saliva testing has emerged as a particularly valuable diagnostic tool, revealing information about bacterial composition, pH levels, and enzymatic activity. This data allows dental professionals to predict which patients are most susceptible to specific conditions and adjust treatment protocols accordingly, creating truly personalised preventive strategies.
Lifestyle Integration and Behavioural Modifications
Nutritional Counselling
Personalised oral health strategies extend beyond the dental surgery to encompass comprehensive lifestyle modifications. Nutritional counselling tailored to individual dietary preferences and cultural backgrounds helps patients make sustainable changes that support oral health. Rather than imposing restrictive dietary rules, modern approaches focus on practical modifications that patients can realistically maintain long-term.
Stress Management and Oral Health
The connection between stress and oral health has gained significant recognition, with personalised strategies addressing individual stress triggers and coping mechanisms. Some patients benefit from night guards to prevent grinding, whilst others require techniques for managing dry mouth caused by anxiety medications. These customised dental treatment approaches acknowledge the whole person rather than focusing solely on oral symptoms.
Long-term Benefits and Cost Effectiveness
Whilst personalised oral health strategies may require greater initial investment in terms of time and diagnostic procedures, they consistently demonstrate superior long-term outcomes. Patients experience fewer emergency interventions, reduced treatment complexity, and improved overall oral health satisfaction. The preventive nature of personalised care often translates to significant cost savings over time, as early intervention proves far more economical than extensive restorative treatments.
Furthermore, individualised dental care plans typically result in higher patient compliance rates, as treatments align more closely with personal preferences and lifestyle requirements. This improved adherence creates a positive cycle of better outcomes and increased patient satisfaction.
Embracing the Future of Oral Healthcare
The evolution towards personalised oral health strategies represents a paradigm shift that benefits both patients and practitioners. By acknowledging individual differences and tailoring treatments accordingly, dental professionals can achieve remarkable improvements in patient outcomes whilst building stronger, more collaborative relationships. As technology continues advancing and our understanding of oral health complexity deepens, personalised approaches will undoubtedly become the gold standard for comprehensive dental care.
HEALTH
gingivitis vs periodontitis: Understanding the Key Differences, Symptoms, and Treatments
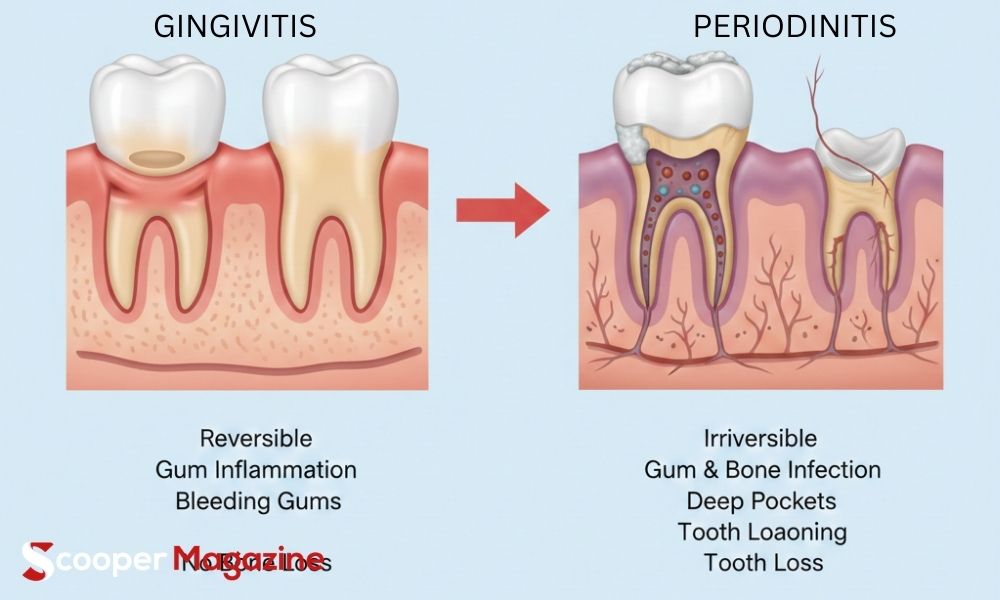
 If you’ve ever noticed bleeding gums while brushing, you may have wondered: Is this just gingivitis, or something more serious like periodontitis?
If you’ve ever noticed bleeding gums while brushing, you may have wondered: Is this just gingivitis, or something more serious like periodontitis?
Understanding gingivitis vs periodontitis is essential for protecting your oral health. While both conditions affect the gums, they are not the same and knowing the difference can literally save your teeth.
In this SEO-optimized and human-friendly guide, we’ll cover:
-
What is gingivitis?
-
What is periodontitis?
-
Key differences between gingivitis vs periodontitis
-
Causes and risk factors
-
Symptoms to watch for
-
Stages of gum disease
-
Treatment options
-
Prevention tips
-
Frequently asked questions
Let’s break it down clearly and simply.
What Is Gingivitis?
Gingivitis is the earliest and mildest form of gum disease. It occurs when plaque — a sticky film of bacteria — builds up on teeth and irritates the gums.
Common signs of gingivitis include:
-
Red or swollen gums
-
Bleeding while brushing or flossing
-
Tender gum tissue
-
Mild bad breath
The good news? Gingivitis is reversible.
With proper oral hygiene and professional dental cleaning, gum tissue can return to a healthy state.
What Is Periodontitis?
Periodontitis is a more advanced and serious form of gum disease. It develops when untreated gingivitis progresses deeper into the gum and bone structures that support the teeth.
Unlike gingivitis, periodontitis can cause permanent damage.
Symptoms of periodontitis may include:
-
Persistent bad breath
-
Gum recession (gums pulling away from teeth)
-
Deep pockets between teeth and gums
-
Loose teeth
-
Pain while chewing
-
Bone loss
Periodontitis is not fully reversible, but it can be managed with professional treatment.
Gingivitis vs Periodontitis: The Key Differences
Understanding gingivitis vs periodontitis becomes easier when you compare them directly.
| Feature | Gingivitis | Periodontitis |
|---|---|---|
| Severity | Mild | Advanced |
| Reversible? | Yes | No (damage is permanent) |
| Bleeding Gums | Common | Common |
| Bone Loss | No | Yes |
| Gum Recession | Rare | Common |
| Tooth Loss Risk | Low | High |
| Treatment | Cleaning & hygiene | Deep cleaning, surgery possible |
The biggest difference in gingivitis vs periodontitis is tissue and bone damage.
Gingivitis affects only the gums.
Periodontitis affects gums, connective tissue, and bone.
What Causes Gingivitis and Periodontitis?
The primary cause of both conditions is plaque buildup.
When plaque is not removed:
-
It hardens into tartar (calculus).
-
Bacteria multiply.
-
The immune system responds with inflammation.
-
Tissue damage begins.
Other contributing risk factors include:
-
Poor oral hygiene
-
Smoking
-
Diabetes
-
Hormonal changes
-
Genetic predisposition
-
Stress
-
Certain medications
Ignoring early gum inflammation increases the risk of progression from gingivitis to periodontitis.
Symptoms: How to Tell the Difference
Many people search “gingivitis vs periodontitis symptoms” because early signs can look similar.
Signs You Likely Have Gingivitis
-
Bleeding when brushing
-
Puffy gums
-
Mild redness
-
No loose teeth
-
No deep gum pockets
Signs You May Have Periodontitis
-
Gums pulling away from teeth
-
Persistent bad breath
-
Teeth shifting position
-
Pus between gums and teeth
-
Pain when chewing
-
Noticeable tooth mobility
If symptoms go beyond mild bleeding, it’s important to consult a dentist.
Stages of Gum Disease
Gum disease typically progresses through stages:
1. Healthy Gums
Firm, pink tissue with no bleeding.
2. Gingivitis
Inflammation without bone damage.
3. Early Periodontitis
Minor bone loss begins.
4. Moderate Periodontitis
Increased bone destruction and pocket formation.
5. Advanced Periodontitis
Severe bone loss, loose teeth, potential tooth loss.
The earlier it’s caught, the easier it is to treat.
Treatment Options: Gingivitis vs Periodontitis
Gingivitis Treatment
-
Professional dental cleaning
-
Improved brushing and flossing routine
-
Antibacterial mouthwash
-
Regular checkups
With proper care, gums can fully heal.
Periodontitis Treatment
Treatment is more complex and may include:
-
Scaling and root planing (deep cleaning)
-
Antibiotic therapy
-
Gum surgery
-
Bone grafting
-
Laser therapy
-
Ongoing periodontal maintenance
Early intervention greatly improves outcomes.
Why Gingivitis Should Never Be Ignored
Many people dismiss bleeding gums as normal.
It’s not.
Bleeding is a sign of inflammation — and untreated inflammation can progress into periodontitis.
The transition from gingivitis to periodontitis often happens gradually and painlessly, which makes regular dental checkups essential.
Prevention: Protecting Your Gum Health
Preventing both gingivitis and periodontitis comes down to consistent habits.
Daily Oral Care
-
Brush twice daily for two minutes
-
Floss once daily
-
Use fluoride toothpaste
-
Consider antimicrobial mouthwash
Professional Care
-
Dental checkups every six months
-
Professional cleanings
-
Periodontal evaluations if needed
Lifestyle Changes
-
Stop smoking
-
Manage diabetes
-
Maintain a balanced diet
-
Reduce stress
Prevention is always easier than treatment.
Long Term Risks of Periodontitis
Advanced periodontitis doesn’t only affect your teeth.
Research links severe gum disease to:
-
Heart disease
-
Stroke
-
Diabetes complications
-
Respiratory infections
-
Pregnancy complications
Oral health is connected to overall health.
Final Thoughts on Gingivitis vs Periodontitis
When comparing gingivitis vs periodontitis, the difference comes down to severity and permanence.
Gingivitis:
-
Mild
-
Reversible
-
Limited to gums
Periodontitis:
-
Serious
-
Irreversible damage
-
Affects bone and connective tissue
The most important takeaway?
Bleeding gums are not “normal.” They are a warning sign.
Addressing gingivitis early prevents it from progressing into periodontitis and potentially saving your smile.
FAQs Gingivitis vs Periodontitis
Is gingivitis painful?
Usually no. It often causes mild discomfort but not severe pain.
Can gingivitis turn into periodontitis?
Yes, if left untreated.
Can periodontitis be cured?
It cannot be fully reversed, but it can be controlled with professional care.
How long does it take for gingivitis to become periodontitis?
It varies depending on oral hygiene, health factors, and genetics.
Is bleeding gums always gingivitis?
Most commonly yes, but a dentist should evaluate persistent bleeding.
HEALTH
why does ozdikenosis kill you? A Complete Scientific and Educational Breakdown
 In recent months, the term ozdikenosis has started appearing across online forums, digital communities, and health-related discussions. Many people are asking the same urgent question:
In recent months, the term ozdikenosis has started appearing across online forums, digital communities, and health-related discussions. Many people are asking the same urgent question:
Why does ozdikenosis kill you?
Before going deeper, it’s important to clarify something essential: Ozdikenosis is not currently recognized in established medical literature as an officially classified disease. It does not appear in standard diagnostic manuals or global health databases.
However, when people search for this phrase, they are typically looking for one of three things:
-
An explanation of a rumored or emerging disease
-
A fictional or hypothetical medical condition
-
A misunderstanding or misinterpretation of another illness
This article will approach the topic from an educational and scientific perspective, explaining how serious diseases kill the body, what mechanisms cause fatal outcomes, and how to evaluate health information responsibly.
If ozdikenosis were a real condition, what biological processes would cause it to become deadly? Let’s explore the science.
How Diseases Kill the Human Body: The Core Mechanisms
To understand why any illness becomes fatal, we must understand how the body maintains life.
Your survival depends on:
-
Oxygen circulation
-
Brain function
-
Heart activity
-
Organ stability
-
Immune balance
When a disease disrupts one or more of these systems severely, death can occur.
Here are the primary mechanisms through which illnesses become fatal.
1. Organ Failure
One of the most common causes of death from illness is organ failure.
Major organs include:
-
Heart
-
Lungs
-
Brain
-
Liver
-
Kidneys
If a disease damages one of these organs beyond recovery, the body can no longer maintain balance.
For example:
-
Respiratory failure prevents oxygen delivery
-
Heart failure stops circulation
-
Liver failure leads to toxin buildup
-
Kidney failure disrupts fluid and electrolyte balance
If ozdikenosis were fatal, it would likely involve progressive organ damage.
2. Severe Infection and Sepsis
Another life-threatening pathway is systemic infection.
When harmful bacteria, viruses, or toxins spread through the bloodstream, the immune system may respond aggressively. In extreme cases, this leads to sepsis, a condition where inflammation becomes widespread and dangerous.
Sepsis can cause:
-
Low blood pressure
-
Multi-organ failure
-
Shock
-
Death
If ozdikenosis involved infectious spread, sepsis could be the fatal mechanism.
3. Oxygen Deprivation (Hypoxia)
Every cell in the body needs oxygen.
If a condition interferes with breathing, blood flow, or oxygen exchange, tissues begin to die. The brain is particularly sensitive permanent damage can begin within minutes.
Diseases that affect:
-
Lungs
-
Blood vessels
-
Hemoglobin function
Can lead to fatal hypoxia.
4. Neurological Shutdown
The brain controls:
-
Breathing
-
Heart rate
-
Consciousness
-
Reflexes
If a disease attacks the nervous system, especially the brainstem, it can disrupt automatic life-sustaining functions.
Severe neurological damage is often irreversible.
5. Immune System Overreaction
Sometimes the immune system itself becomes the problem.
In certain diseases, the immune response becomes exaggerated, causing a “cytokine storm.” This intense inflammatory reaction can damage tissues and organs.
This is not uncommon in severe viral infections.
Hypothetical Progression of a Fatal Disease Like Ozdikenosis
If ozdikenosis were structured as a progressive disease, it might follow stages similar to other systemic conditions.
Stage 1: Early Symptoms
-
Fatigue
-
Fever
-
Mild discomfort
-
Headaches
-
Muscle weakness
At this stage, symptoms might seem manageable.
Stage 2: Systemic Spread
The illness begins affecting:
-
Circulatory system
-
Respiratory function
-
Immune balance
Symptoms worsen:
-
Persistent fever
-
Breathing difficulty
-
Chest discomfort
-
Cognitive changes
Stage 3: Organ Complications
At this stage:
-
Oxygen delivery may decline
-
Blood pressure may drop
-
Inflammation increases
Without intervention, organ damage becomes severe.
Stage 4: Critical Failure
The final stage might involve:
-
Multi-organ failure
-
Shock
-
Cardiac arrest
-
Brain dysfunction
This is how many severe diseases ultimately become fatal.
Risk Factors That Make Illnesses Deadlier
Whether discussing real diseases or hypothetical ones, fatality risk increases when individuals have:
-
Weakened immune systems
-
Chronic illnesses
-
Advanced age
-
Delayed treatment
-
Poor nutrition
-
Lack of medical access
Early detection often makes the difference between recovery and fatal outcome.
The Importance of Accurate Medical Information
Because ozdikenosis is not recognized in medical literature, it is critical to avoid spreading misinformation.
In today’s digital environment, viral health terms can spread rapidly through:
-
Social media
-
Online forums
-
Short-form videos
-
Unverified blog posts
Always verify health information through:
-
Licensed healthcare professionals
-
Established medical institutions
-
Peer-reviewed research
Misinformation can cause unnecessary fear or delay proper treatment for real conditions.
Psychological Impact of Searching Fatal Disease Terms
When people search “why does ozdikenosis kill you,” it often reflects anxiety about health.
Health related fear is common, especially in an era of instant online access to alarming information.
If you are experiencing:
-
Persistent worry about unknown diseases
-
Anxiety about symptoms
-
Fear triggered by online content
It may help to consult a medical professional rather than relying on unverified digital discussions.
How Real Diseases Are Diagnosed
Legitimate diseases are identified through:
-
Clinical symptoms
-
Laboratory testing
-
Imaging scans
-
Biopsy (in some cases)
-
Scientific classification
If a condition lacks medical documentation, it should be approached cautiously.
Preventing Severe Illness in General
While ozdikenosis is not medically recognized, preventing severe disease in general includes:
-
Regular health checkups
-
Vaccinations (where appropriate)
-
Healthy diet
-
Adequate sleep
-
Exercise
-
Stress management
-
Avoiding tobacco
-
Limiting alcohol
Strong immune health reduces vulnerability to many conditions.
Could Ozdikenosis Be a Misunderstood Term?
Sometimes unfamiliar medical-sounding words emerge from:
-
Misspellings
-
Fictional content
-
Online hoaxes
-
Viral jokes
-
Misinterpretation of scientific terminology
Before assuming a disease is real, check:
-
Medical databases
-
Government health sites
-
Trusted hospital resources
When to Seek Medical Attention
Regardless of terminology, seek immediate medical care if you experience:
-
Severe chest pain
-
Difficulty breathing
-
Sudden confusion
-
Persistent high fever
-
Fainting
-
Uncontrolled bleeding
These symptoms require urgent evaluation.
Why Fear-Based Health Content Spreads Quickly
Content about fatal diseases spreads because it triggers:
-
Survival instinct
-
Curiosity
-
Emotional response
-
Social sharing
However, viral content does not equal medical accuracy.
Critical thinking is essential.
Final Thoughts: Why Does Ozdikenosis Kill You?
Based on current medical knowledge, ozdikenosis is not a recognized medical condition.
Therefore, there is no scientifically verified explanation for how it kills.
However, understanding how real diseases become fatal helps answer the broader question.
Diseases kill by:
-
Causing organ failure
-
Disrupting oxygen flow
-
Triggering systemic infection
-
Damaging the brain
-
Creating uncontrolled inflammation
If you encounter alarming health terms online, verify them before assuming danger.
Knowledge, not fear, is the best defense against misinformation.
FAQs
1. Is ozdikenosis a real disease?
There is no verified medical evidence that ozdikenosis exists as a recognized illness.
2. Why are people searching for ozdikenosis?
It may be trending online due to misinformation, fictional content, or misunderstanding.
3. How do real diseases kill people?
Through organ failure, infection, oxygen deprivation, or neurological damage.
4. Should I be worried about ozdikenosis?
There is currently no scientific basis for concern.
5. What should I do if I feel sick?
Consult a licensed healthcare provider for accurate diagnosis and treatment.
HEALTH
timeshealthmag nutrition: Your Complete Guide to Smart Eating

 Introduction: What Is TimesHealthMag Nutrition?
Introduction: What Is TimesHealthMag Nutrition?
In today’s fast-paced world, maintaining a healthy diet can feel overwhelming. With conflicting advice everywhere, people often struggle to determine what truly supports long-term wellness. That’s where TimesHealthMag Nutrition comes in.
TimesHealthMag Nutrition focuses on practical, science-backed dietary guidance designed for modern lifestyles. Instead of promoting extreme diets or unrealistic food restrictions, it encourages balanced eating, mindful habits, and sustainable health improvements.
In 2026, nutrition is no longer just about counting calories — it’s about understanding how food affects energy, immunity, mental clarity, and long-term disease prevention.
Why Nutrition Matters More Than Ever
Good nutrition is the foundation of overall health. The food we eat directly impacts:
-
Energy levels
-
Brain function
-
Immune system strength
-
Hormonal balance
-
Weight management
-
Heart health
TimesHealthMag Nutrition emphasizes that proper nutrition is not about perfection. It’s about making consistent, informed choices that support your body over time.
Poor dietary habits can lead to chronic conditions such as obesity, diabetes, cardiovascular disease, and digestive disorders. However, small improvements in daily eating patterns can significantly reduce these risks.
Core Principles of TimesHealthMag Nutrition
TimesHealthMag Nutrition is built around simple but powerful principles:
1. Balance Over Restriction
Instead of eliminating entire food groups, focus on balanced meals that include proteins, healthy fats, complex carbohydrates, vitamins, and minerals.
2. Whole Foods First
Minimally processed foods provide better nutrients compared to highly processed alternatives. Fresh vegetables, fruits, lean proteins, whole grains, and nuts are encouraged.
3. Portion Awareness
Portion control helps maintain healthy weight without extreme dieting.
4. Hydration Matters
Drinking enough water is essential for digestion, metabolism, and detoxification.
5. Sustainability
Healthy eating should be realistic and maintainable long-term.
Essential Nutrients for Optimal Health
Understanding nutrients is key to smart eating.
Macronutrients
Protein
Supports muscle repair, immune function, and satiety.
Sources: Lean meats, fish, beans, tofu, eggs.
Carbohydrates
Provide energy. Choose complex carbs like whole grains over refined sugars.
Healthy Fats
Important for brain health and hormone production.
Sources: Avocados, olive oil, nuts, seeds.
Micronutrients
Vitamins
Support immune function, bone health, and energy production.
Minerals
Calcium, iron, magnesium, and potassium are essential for various body functions.
TimesHealthMag Nutrition promotes a colorful plate — the more natural colors in your meals, the broader the nutrient range.
Popular Nutrition Trends in 2026
Nutrition trends evolve every year. According to TimesHealthMag Nutrition insights, here are key trends shaping healthy eating:
1. Plant-Forward Diets
More people are incorporating plant-based meals without fully eliminating animal products.
2. Gut Health Focus
Probiotics and fiber-rich foods are gaining attention for digestive wellness.
3. Personalized Nutrition
DNA testing and AI-driven meal plans are becoming more common.
4. Clean Label Products
Consumers prefer food products with transparent ingredient lists.
How to Build a Balanced Meal
A simple formula recommended by TimesHealthMag Nutrition:
-
½ plate vegetables
-
¼ plate lean protein
-
¼ plate whole grains
-
Add healthy fats
-
Include water or herbal tea
This structure ensures balanced macronutrients and fiber intake.
Weight Management and Nutrition
Healthy weight management is about habits, not crash diets.
Tips include:
-
Avoid skipping meals
-
Eat mindfully
-
Reduce added sugars
-
Prioritize protein and fiber
-
Get enough sleep
TimesHealthMag Nutrition stresses that consistency matters more than short-term dieting.
Nutrition for Mental Health
Food affects mood and mental clarity. Diets rich in omega-3 fatty acids, antioxidants, and B vitamins support cognitive function.
Highly processed foods and excessive sugar intake can negatively impact mental well-being.
Eating balanced meals stabilizes blood sugar, which improves focus and reduces mood swings.
Common Nutrition Mistakes to Avoid
-
Over-restricting calories
-
Ignoring hydration
-
Relying on supplements instead of whole foods
-
Following social media diet trends blindly
-
Skipping breakfast regularly
TimesHealthMag Nutrition encourages evidence-based guidance over viral trends.
Practical Daily Nutrition Tips
-
Plan meals in advance
-
Keep healthy snacks available
-
Read food labels
-
Cook more at home
-
Practice mindful eating
Small daily improvements create long-term results.
The Role of Supplements
Supplements can support nutrition but should not replace balanced meals.
Common supplements include:
-
Vitamin D
-
Omega-3
-
Multivitamins
-
Magnesium
Consulting a healthcare professional before supplementation is recommended.
Nutrition and Long-Term Health
A nutrient-rich diet reduces the risk of:
-
Heart disease
-
Type 2 diabetes
-
Obesity
-
Certain cancers
TimesHealthMag Nutrition promotes preventive health through consistent dietary choices.
Final Thoughts
TimesHealthMag Nutrition promotes a realistic and balanced approach to healthy eating in 2026. Rather than extreme restrictions, it emphasizes consistency, whole foods, hydration, and mindful habits.
Good nutrition is not about short-term results it is about building a lifestyle that supports long-term health, energy, and overall well-being.
Frequently Asked Questions
1. What is TimesHealthMag Nutrition?
TimesHealthMag Nutrition provides guidance and insights focused on balanced eating, wellness, and sustainable dietary habits.
2. Is calorie counting necessary?
Not always. Focusing on whole foods and portion awareness can be more sustainable.
3. Can I enjoy treats occasionally?
Yes. Moderation is key to maintaining a healthy relationship with food.
4. How much water should I drink daily?
Most adults benefit from 2–3 liters per day, depending on activity level.
5. Is a plant-based diet required?
No. Balanced nutrition can include both plant and animal-based foods.
-

 TECH2 months ago
TECH2 months agoanonposted Explained: Features, Privacy, Uses, and What Users Should Know
-

 CELEBRITY1 year ago
CELEBRITY1 year agoWho Is Amelia Jane Henson? Everything You Need to Know About Mia Sara and Brian Henson’s Daughter
-

 BUSINESS1 year ago
BUSINESS1 year agoWho Is Nadia Farmiga? Everything You Need to Know About Vera Farmiga’s Sister
-

 CELEBRITY1 year ago
CELEBRITY1 year agoWho Is Jasmine Gong? Everything You Should Know About Brad Williams’ Wife
-

 CELEBRITY1 year ago
CELEBRITY1 year agoWho Is Rosemary Margaret Hobor?: Everything You Need to Know About John Candy’s Wife
-

 CELEBRITY1 year ago
CELEBRITY1 year agoMatt Danzeisen: The Influential Yet Low-Key Force Behind Peter Thiel’s Success
-

 CELEBRITY1 year ago
CELEBRITY1 year agoRachel Catudal: Everything You Need to Know About Brandon Quinn’s Wife
-

 CELEBRITY1 year ago
CELEBRITY1 year agoWho Is Gianluca Cugnetto? Everything You Need to Know About Hannah Waddingham’s Ex-Husband



